Peroneal Tendon Subluxation
Read More >
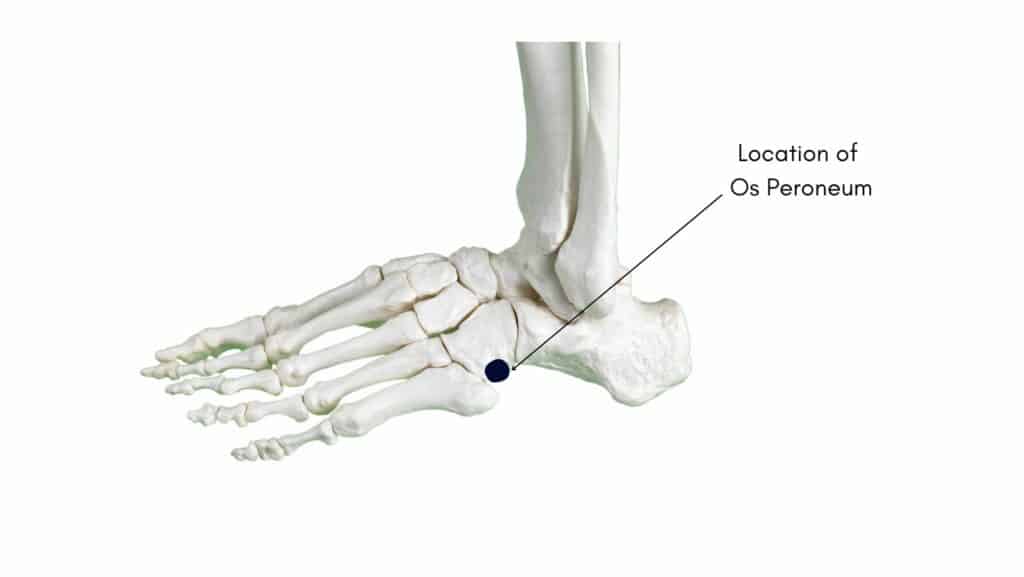
An Os Peroneum is an accessory bone found in the Peroneus Longus Tendon on the outer aspect of the midfoot of approximately 20-30% of the population. There is no known mechanical benefit of this extra bone, and in most instances, people go their whole lives without knowing they have an Os Peroneum. However, if the Os Peroneum becomes overloaded or direct stress is placed on it, it can become inflamed and lead to Os Peroneum Syndrome.
The Peroneus Longus tendon is one of 3 primary Peroneal tendons; it runs along the outside of your ankle bone before taking an acute turn at the cuboid tunnel before attaching to the medial foot. The function of the Peroneus Longus is to help turn the foot outwards and downwards while also providing stability to the foot when walking and running. It is at the cuboid fossa that most accessory Os Peroneum bones are found.
Trauma, ankle sprains and repetitive strain can cause pain in the Os Peroneum and in severe cases, this can lead to a fracture. Throughout the article, we will explore these causes, explain how to diagnose a painful Os Peroneum Syndrome and provide recommended treatment options.
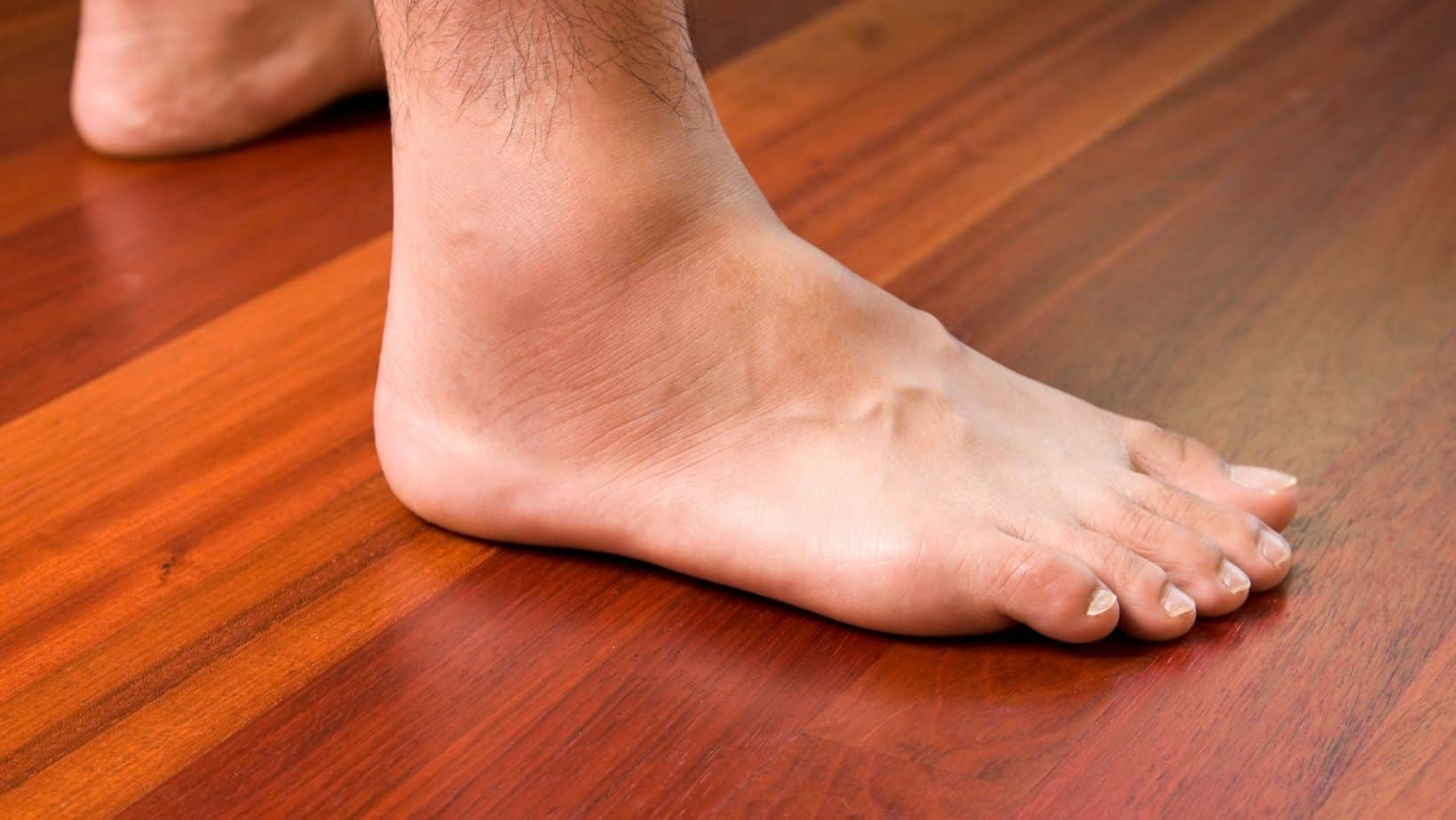
The symptoms of Os Peroneum Syndrome include pain and swelling on the lateral (outer) aspect of the foot that can cause visible swelling and redness. These may be more prominent if the injury develops into a stress fracture.
Walking barefoot, on uneven surfaces or wearing unsupportive footwear can aggravate the symptoms of Os Peroneum Syndrome. The outer aspect of the foot around the Cuboid Bone is often tender to touch, while turning the foot outwards can exacerbate the symptoms of Os Peroneum Syndrome.
As injury to the Os Peroneum often occurs after an ankle sprain, there can be general discomfort of the entire outer ankle and foot while a sprain may lead to a tear in the Peroneus Longus, causing the Os Peroneum to move away from the Cuboid fossa and closer to the ankle joint.
Os Peroneum syndrome is often misdiagnosed as other common conditions of the outer foot, such as Peroneal Tendonitis, 5th metatarsal fracture or a cuboid fracture.
Os Peroneum Syndrome is caused by trauma or overload to the Os Peroneum or overuse of the Peroneus Longus Tendon.
Trauma can directly impact the Os Peroneum, resulting in a bone fracture of the bone while a severe ankle sprain can irritate the Os Peroneum.
Poorly supported footwear or repetitive impact can lead to overload and overuse of the Os Peroneum to cause Os Peroneum Syndrome, while we often see this in dancers and gymnasts.
Finally, a Peroneus Longus tear can result in a distal fracture of an Os Peroneum.
A Physical Assessment by a Physical Therapist or a Sports Medicine Doctor can identify potential Os Peroneum Syndrome, but imaging is usually required to confirm the diagnosis.
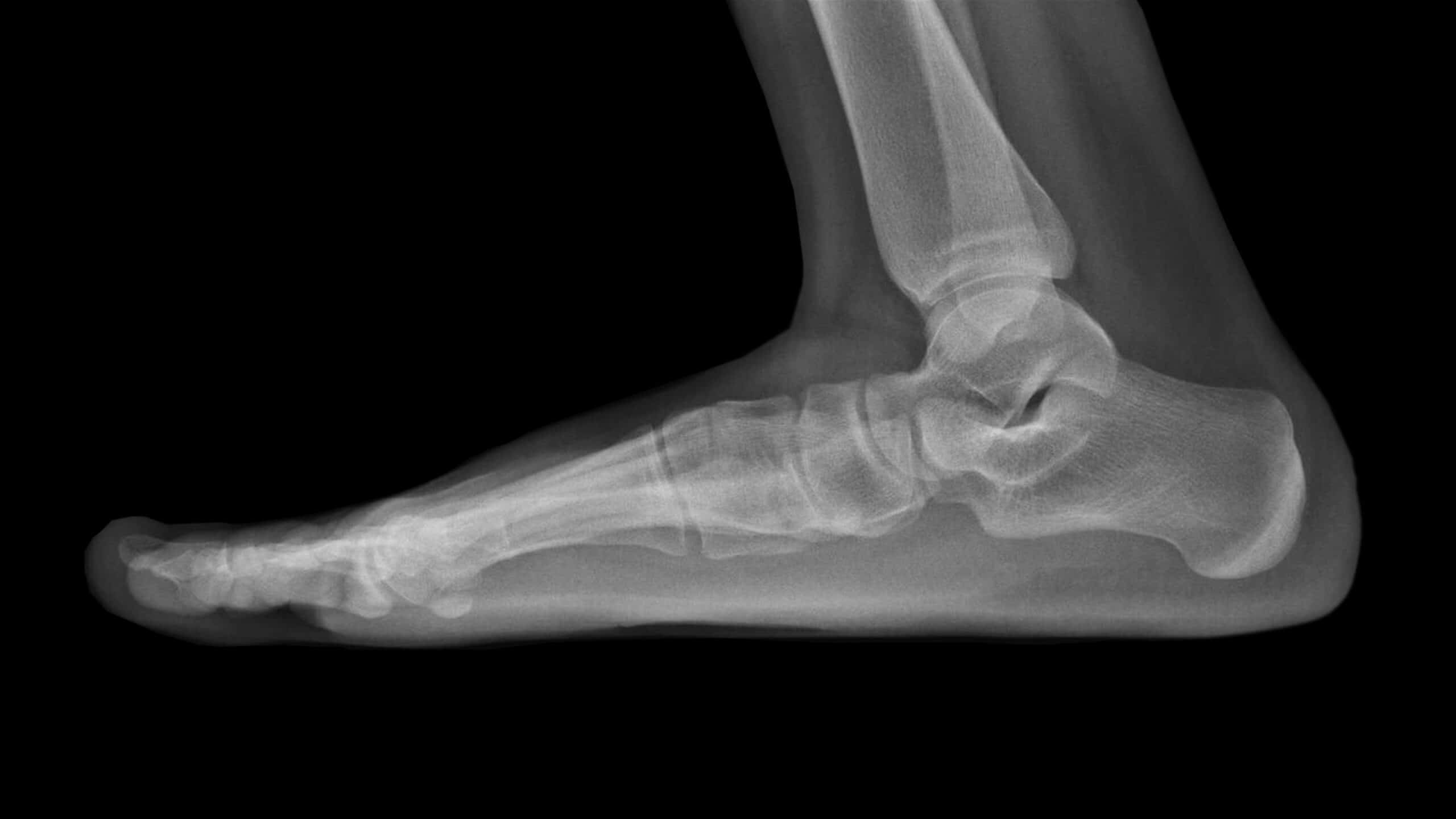
An ultrasound scan can identify an Os Peroneum, while an x-ray is also a cost-effective diagnostic tool.
An x-ray can identify the presence of a bi-partite Os Peroneum, a non-displaced or displaced fracture.
An MRI can rule out other conditions that can cause extreme foot pain.
In most cases of Os Peroneum Syndrome, ice, rest and anti-inflammatories can be sufficient to calm down the symptoms before increasing function levels.
In some cases, a walker boot is required to reduce inflammation, and a Physical Therapist can guide a patient through how to transition from a walker boot to an everyday shoe. A therapist may tape the ankle into slight eversion as it shortens the Peroneal Tendons to reduce the strain on the outer foot when walking or standing.
It is important to remember that these steps are recommended to alleviate the symptoms of Os Peroneum Syndrome. Still, it is important to address biomechanical factors that may be causing the overload of this accessory bone.
During this process, strengthening and mobility exercises are beneficial to address biomechanical issues that may be overloading the outer aspect of the foot. These exercises are similar to the ones that we have recommended for ankle sprains.
A gait analysis assesses how your feet move as you stand, walk and run, which is beneficial to identifying the need for stability shoes or insoles. These can help to control the movement of the feet or offload the outer foot to reduce your pain levels.
If treatment is unsuccessful, an ultrasound-guided steroid injection may reduce inflammation in the area. There are risks associated with an injection such as a steroid flare or infection. The injection takes up to two weeks to take effect. During this time, you may be recommended to spend time in a walker boot to allow the injection to take maximum effect before recommencing rehabilitation.
While surgery is rare, it can involve removing the bone or repairing the Peroneus Longus Tendon.
This is not medical advice; you should consult your healthcare practitioners if you have any of the symptoms mentioned in this article. We recommend consulting with a medical professional such as James McCormack if you have foot or ankle pain. James offers Online Physiotherapy Appointments.