Bunion Boot
Read More >
A Bunion or Hallux Limitus refers to a change in the angulation of the joint of the big toe, causing the big toe to deviate away from the midline and towards the 2nd-5th toes.
The long bone before the big toe is known as the 1st Metatarsal, and the bone of the big toe is known as a Phalanx. The point where these bones meet is the Metatarsophalangeal Joint (MTP). The MTP joint is the site of the typical bump on the side of the foot that most people associate with a bunion.
Bunions can be hereditary, with some studies finding that up to 90% of people with bunions have a family history of bunion formation. Bunions are more common in females and more prevalent in the older population. In some cases, a bunion can be completely pain-free despite a considerable change in the normal position of the MTP, while others can have extremely painful bunions.
There are different types of bunions: adolescent bunions form between the ages of 10-15 and are often pain-free, while an adult bunion is often stiff and painful. A bunion that forms on the little toe is known as a Bunionette (Tailor’s Bunion).
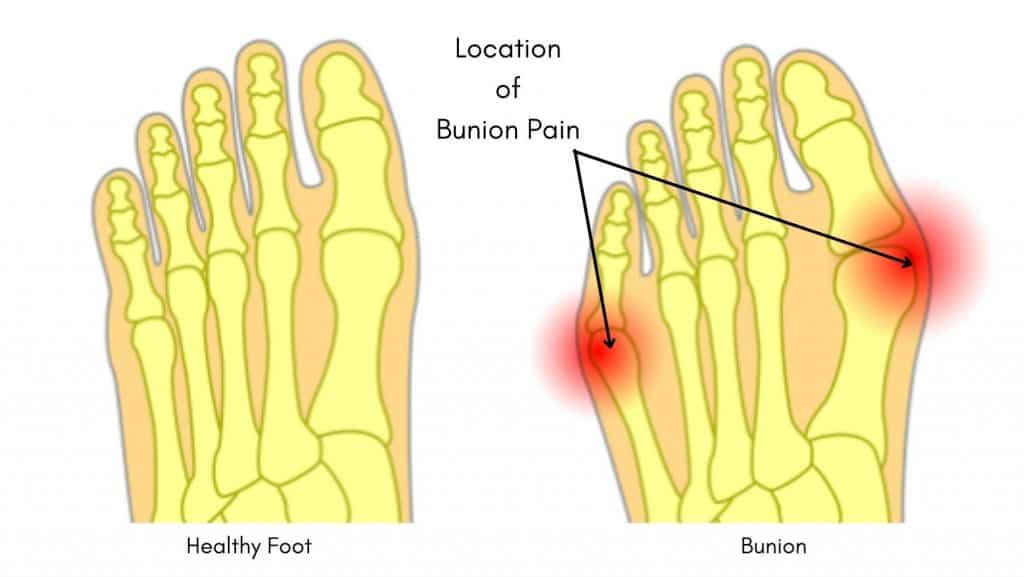
Patients describe bunion symptoms as a burning hot sensation at the base of the big toe. Walking, running, and tip-toe walking can worsen the symptoms of a bunion, as can wearing ill-fitting footwear or high heels.
A bunion is tender to the touch and can be red and swollen when irritable. Bunion pain is worse with activity and should improve with relative rest.
There may be some pins and needles in severe cases where swelling irritates the surrounding nerves. The range of motion of the big toe joint is often less than usual, while callus formation and corns are often present alongside a bunion.
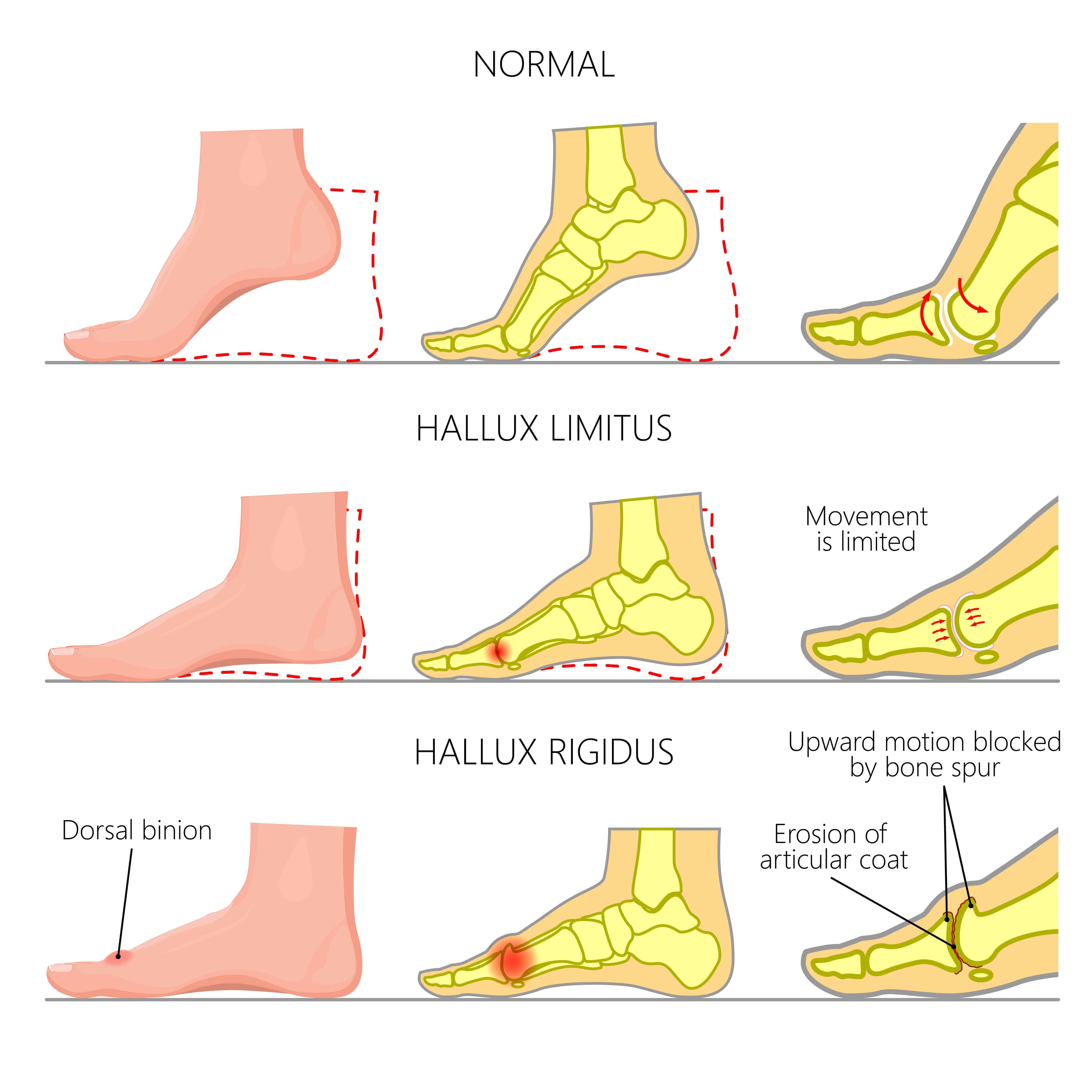
A congenital bunion is formed from birth and is a result of genetics. All other forms of bunions can be caused by altered foot mechanics, ill-fitting shoes where the toe box is too narrow, high heels and trauma such as a fracture to the big toe.
Certain foot types, such as flat feet, can contribute to bunion formation and poor control of pronation moments when running or walking.
Other causes of a bunion include Hallux Rigidis, arthritis and rheumatoid arthritis.
If you have a genetic predisposition to bunions then it is difficult to stop them.
The key factors to consider are optimal footwear, foot strengthening and insoles if necessary.
A bunion can be easily identified in a clinic by a Physical Therapist or a Podiatrist. An essential aspect of the Physical examination is to identify the cause of your bunion and form an elaborate rehabilitation protocol. Sometimes, the clinician may want to rule out other conditions, such as a bone spur.
An X-ray is a cheap and easily resourced scan that can quickly diagnose a bunion, arthritis or a bony spur. An MRI may be requested if the clinician needs further information on the soft tissue to identify a condition such as bursitis.
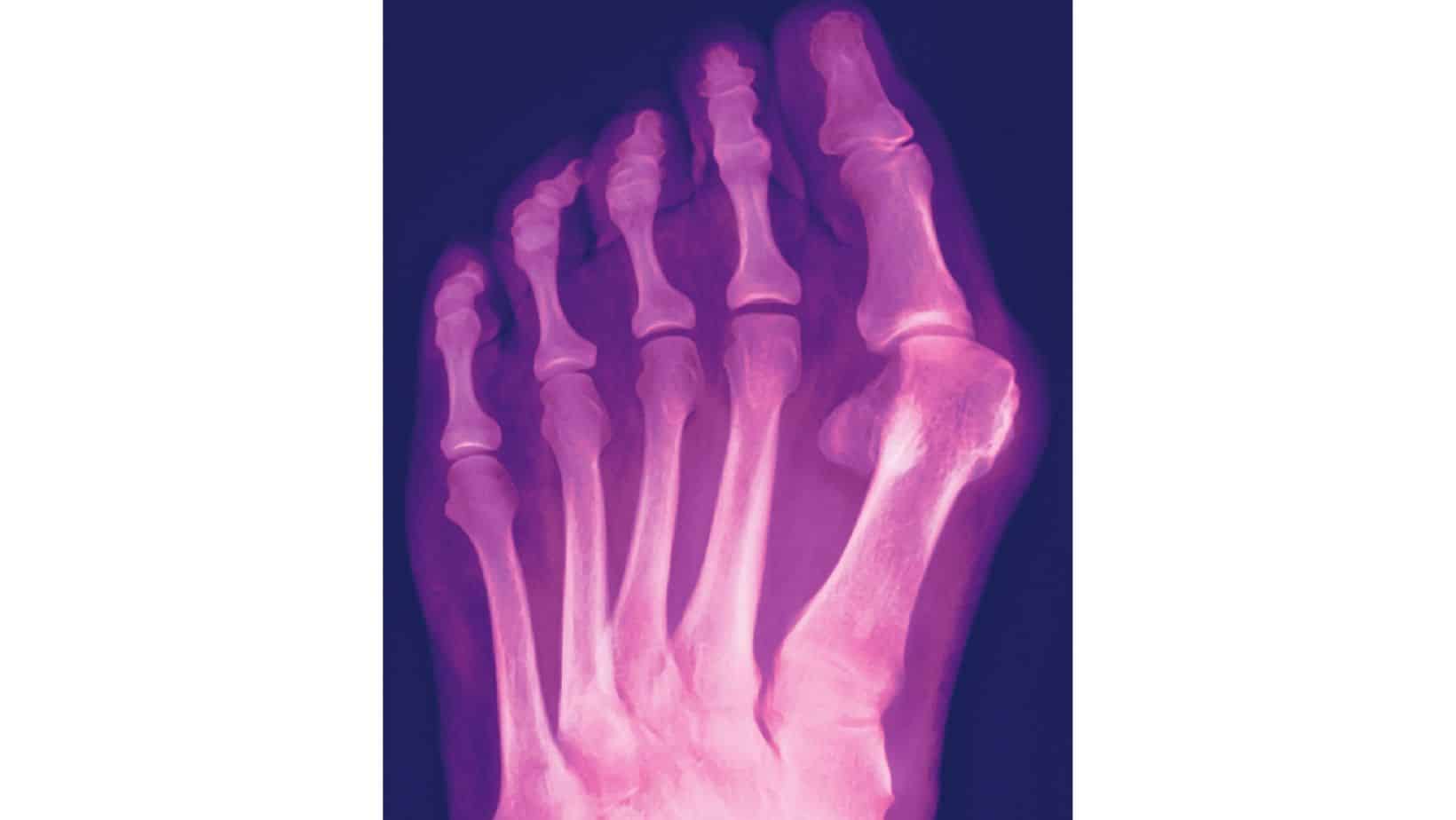
In most cases, home treatment can provide pain relief to those with bunions and is an excellent way to reduce the risk of further deterioration of a bunion.
Home treatment should involve:
Physical therapy is the most effective form of non-surgical treatment for a bunion. Following a Physical Assessment, a discussion around footwear, lifestyle and foot mechanics is imperative.
Bunion taping with KT tape or rigid tape can provide some pain relief alongside mobalisations of the toe and massage to the foot and surrounding muscles. Strengthening exercises and stretches should form the foundations of a rehabilitation protocol.
In some cases, footwear modifications are required, including insoles or orthotics for bunions to offload the big toe and optimise your gait.

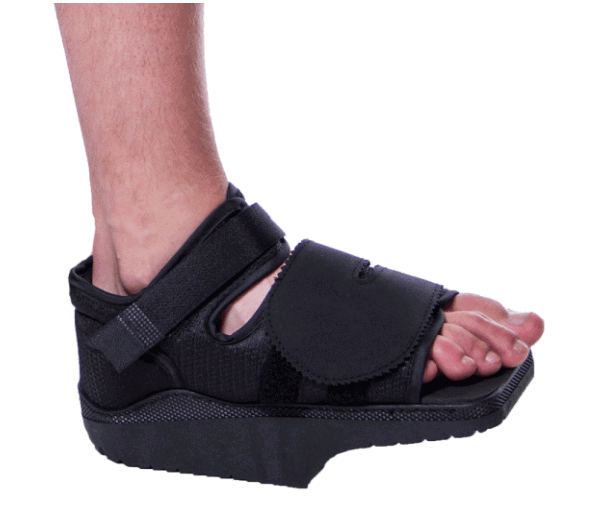
If there is minimal improvement in symptoms, an ultrasound-guided injection can be carried out to reduce inflammation levels in the joint.
Before recommencing Physical Therapy, an injection may be followed by 1-2 weeks in a bunion boot.
If 6-12 weeks of rehabilitation results in minimal to no change in your symptoms, surgery may be recommended, usually in the form of a bunionectomy.
Outcomes for surgery have dramatically improved over the last 10 years. Still, there remains a painful and prolonged recovery period after surgery, so we always recommend exhausting all non-surgical options for at least 3 months before surgery.
If you have an asymptomatic or mild bunion, you can continue running. However, if you have a severe bunion, we recommend that our patients cease running until they have a running gait analysis. This analysis aims to identify factors in your running style that can contribute to the formation and worsening of your bunion. Simple measures like increasing your cadence or foot strike position can prolong your ability to run with a bunion.
Footwear choices are essential when it comes to running with a bunion. Minimalist running shoes have a higher likelihood of irritating symptoms, while cushioned, stable shoes are likely to reduce pain levels and prolong your ability to run with a bunion.
Movement patterns of the foot mainly cause bunions through the gait cycle, flat feet or poor footwear. If your biomechanics make you more susceptible to developing a bunion when walking, then running can do the same but faster due to the increased force associated with running.
Related Article: Best Running Shoes for Bunions
Bunion formations are very slow and progressive unless there has been trauma, such as a fracture to the big toe. Keeping this in mind, if you have no pain or mild pain, you can continue to walk as usual with a bunion.
If you have moderate or severe symptoms of a bunion, you can continue to walk, but consider walking for up to 20 minutes at a time 3-4 times daily rather than lengthy walks of 1 hour or more.
James McCormack, an expert in treating bunion pain, wrote this article.
This is not medical advice. We recommend a consultation with a medical professional such as James McCormack. He offers Online Physiotherapy Appointments weekly and face-to-face appointments in his London clinic.