Posterior Tibial Tendonitis
Read More >
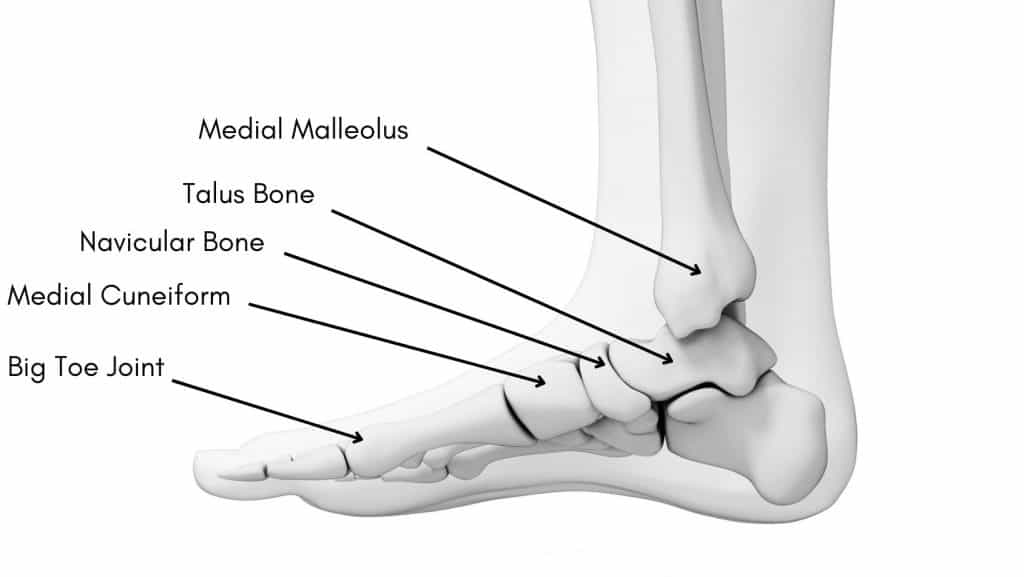
The ankle joint consists of 3 bones: the Tibia, Fibula and Talus. The medial malleolus is the bony prominence on the inner aspect of your ankle joint at the bottom of the tibia.
The medial malleolus is a robust structure that accepts up to 4.7 times your body weight when walking. Therefore, it’s much less common to experience a fracture than a Lateral Malleolus. Still, when they occur, it is usually related to a significant injury involving multiple structures.
This article will explore the different types of Medial Malleolus Fractures and how they are managed.
The symptoms of Medial Malleolus Fractures can vary depending on the type and severity of the break. Overall, there usually is pain inside the ankle with swelling and bruising. It is not unusual for the bruising to seep into the foot due to gravity, and it can be too painful to bear weight.
Walking and running are often painful, with pain easing when non-weight bearing. There may be a throbbing sensation at rest with increased prevalence at night. It usually follows a painful pattern with all weight-bearing activities, unlike a tendon injury that may improve during an activity.
It can be tender to press on the medial malleolus, and the foot position may deform in severe fractures following an ankle dislocation.
This is a common cause of Medial Malleolus Fracture, where a ligament or tendon pulls off a chip or fragment of the bone.
An Avulsion fracture is an isolated Medial Malleolus Fracture and commonly occurs with an ankle sprain where the ligament doesn’t tear but is pulled off the bone instead.
This is normal, a minor fracture to the Medial Malleolus, which is in line with the ankle joint and mainly managed conservatively.
A Medial Malleolus Oblique Fracture usually results from a rotational injury and often involves the fibula bone or other structures, such as an Achilles Tendon rupture.
Most oblique Medial Malleolus Fractures are operated on.
A vertical Medial Malleolus Fracture usually occurs from high forces coming through the ankle joint and is generally stabilised with a plate and screws.
This is a complex fracture involving multiple structures and requires extensive surgery for recovery.

An isolated Medial Malleolus Fracture is one of the most common types of Medial Malleolus Fracture and can be caused if the foot is forcefully turned inwards or outwards.
Repetitive impact without any trauma can cause stress fractures of the Medial Malleolus. This fracture is commonly seen in runners, ballet dancers and gymnasts.
Trauma such as a tackle in a sport, a trip or a fall can also lead to displaced Medial Malleolus Fractures.
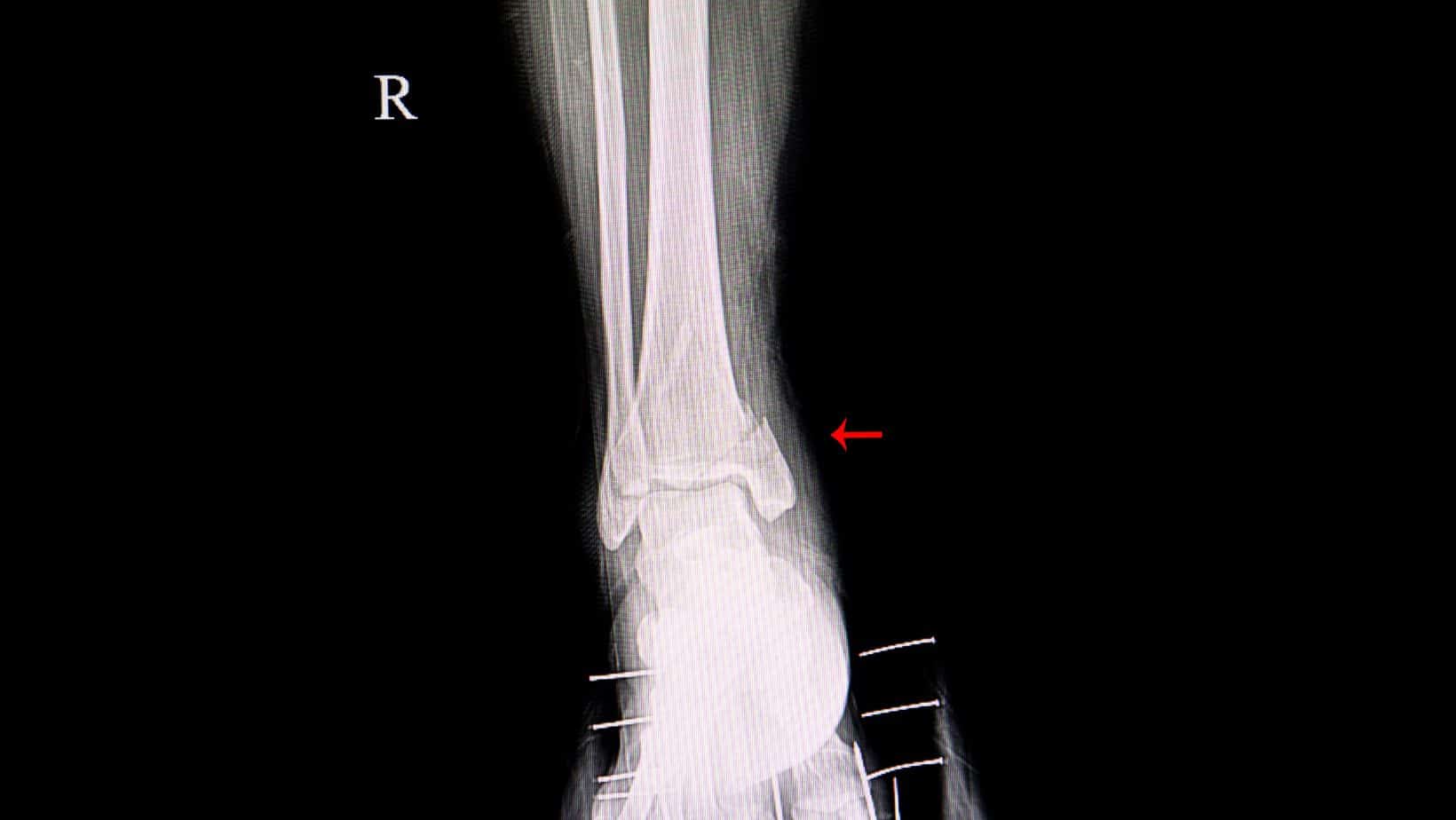
In the first instance, an X-ray is a cost-effective form of imaging to diagnose a Medial Malleolus Fracture.
If there is a lot of swelling in the area, it can make the scan harder to interpret, and usually, a fracture that is a couple of weeks old is easier to identify than an acute fracture.
An MRI can provide more detailed information on a bony injury and soft tissue structures such as ligaments and tendons.
A CT Scan will give the most detailed information on a fracture and is often used to establish the severity of a fracture.
Conservative treatment of Medial Malleolus Avulsion Fractures requires 4-6 weeks in a walker boot. During this period, you can commence Physical Therapy to assist with mobilisation, isometric strengthening exercises and soft tissue work to maintain flexibility in the ankle joint muscles.
Walking in the boot for short distances is allowed, but pain levels should dictate it. You may sometimes be required to bear partial weight using a walking boot before progressing to full weight bearing.
After 4 weeks, it is common to start weaning out of the walker boot, usually indoors with a cushioned trainer, progressing to short walks outdoors. Physical Therapy rehabilitation will become progressively more challenging with stability, balance and strengthening exercises.
If the bone fails to unite, surgery may be required, and for different types of fractures, different forms of stabilisation are required ranging from a screw fixation to an ORIF.
This is not medical advice. We recommend a consultation with a medical professional such as James McCormack. He offers Online Physiotherapy Appointments weekly.