Read More >
- Anterior Ankle Impingement - July 24, 2022
- Tarsal Coalition - October 12, 2022
- Sural Nerve Pain - October 3, 2022
What is a Dislocated Ankle?
The upper aspect of the ankle joint consists of 3 bones; the Talus Bone, Medial and Lateral Malleolus, while the lower aspect, known as the subtalar joint, consists of 2 bones; the Talus bones and the Calcaneus Bone. Ligaments attach bone to bone to help create a joint, and if there is a sudden movement with a change of direction and force, it can lead to one of these bones or more separating from the joint; this is known as an Ankle Dislocation. Commonly when this occurs, there is also a fracture of one of these bones, known as an Ankle Fracture-Dislocation.
Of note, 99% of ankle dislocations are Ankle Fracture-Dislocations.
Dislocated Ankle Symptoms
The symptoms of a Dislocated Ankle include:
- A crack or popping sound
- Immediate onset of intense pain and swelling
- A visible change in the position of the foot
- Inability to move the ankle joint
- Visible protruding of the bone through the skin in open fractures.
- 46% of Ankle Dislocations are posteromedial

Dislocated Ankle Causes
Ankle dislocations are more prevalent in males (72%) that are primarily caused by sports (31%) or motor accidents (30%). When playing sports, the common causes of a dislocated ankle include the foot being fixed in a plantarflexed position and impact to either side of the ankle in a tackle or when landing from a jump (gymnastics and basketball).
A previous history of repetitive ankle sprains can increase your risk of ankle dislocation, as can hypermobile ankles.
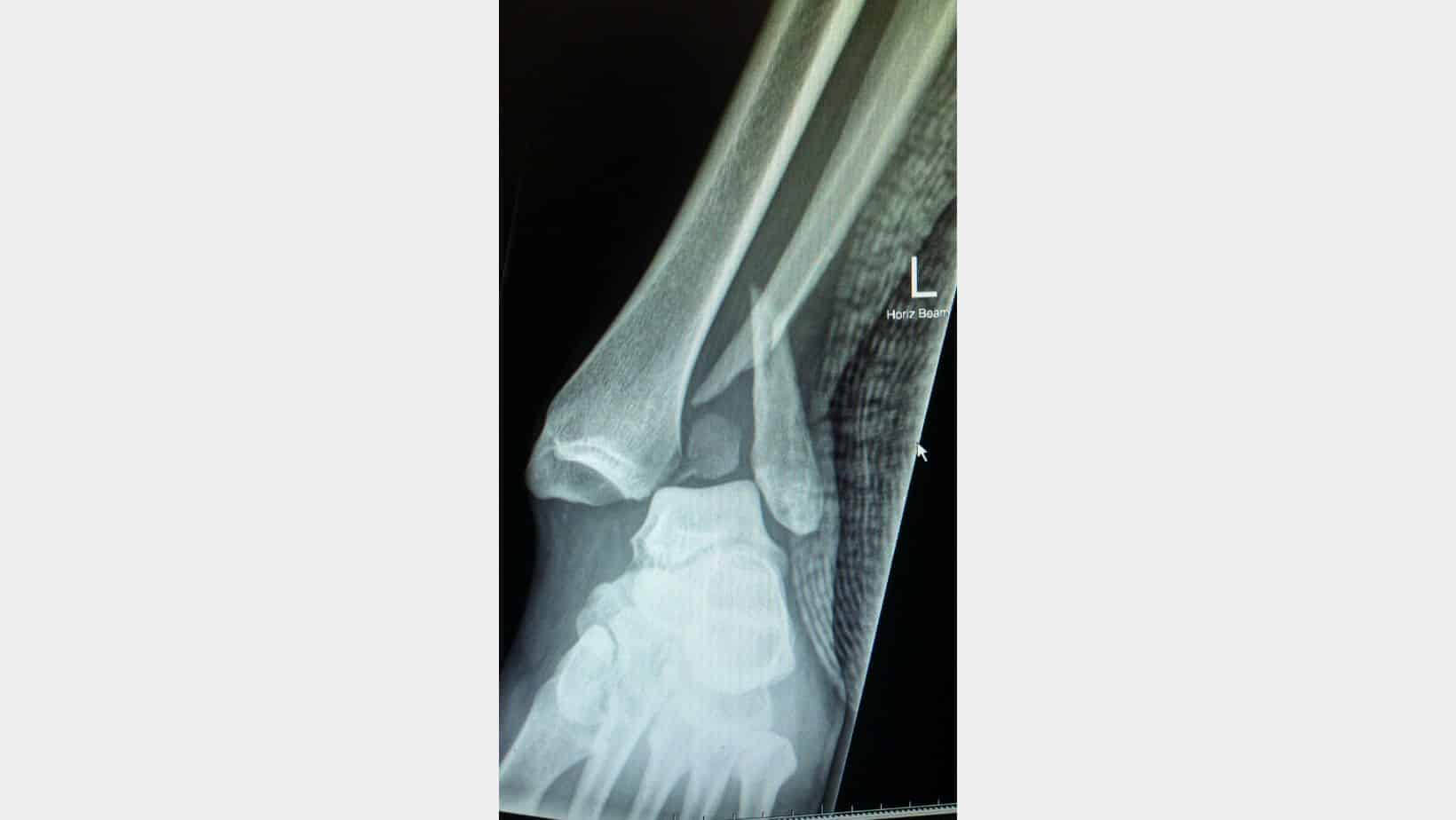
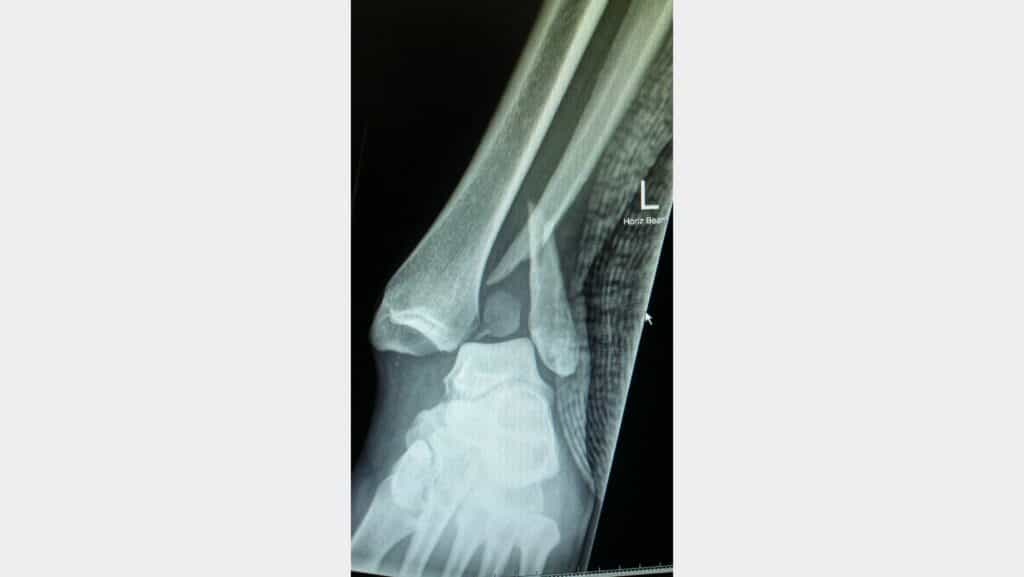
Dislocated Ankle Diagnosis
A diagnosis of a dislocated ankle usually occurs in A&E through an x-ray to determine which bones have been affected and the direction of dislocation. Once relocated, it is common to have an MRI to determine the extent of the injury, including soft tissue damage. At the same time, some cases may require a CT Scan for more detailed images of bone and cartilage condition.
Dislocated Ankle Treatment
There are 5 directions that an ankle can dislocate: anteriorly, posterior, laterally, medially or superiorly in relation to the talus bone on the tibia bone. The anterior, posterior, medial and lateral dislocation can usually be reduced in A&E under sedation, while a superior dislocation requires an MDT consultation to decide on the best treatment. The ankle is usually placed into a splint until an x-ray confirms the anatomical alignment.
Depending on the case, 88% of ankle dislocations are treated conservatively, with some placed in a cast for 6 weeks and others in a walker boot. Once approved by an Orthopaedic Consultant, Physical therapy can be commenced.
In the early stages, manual therapy to assist with soft tissue tightness and reduction of swelling is beneficial alongside hydrotherapy. Isometric strengthening exercises of the ankle and foot muscles can help stimulate the stabilisers of the ankle.
Over 4-6 weeks, a patient will wean out of the walker boot, and some cases require a brace of taping for additional support during this transition. Strengthening exercises will become more dynamic with a mixture of resistance band exercises through the range and progressing into weight-bearing exercises.
Advice on footwear and the need for insoles with your therapist can be beneficial, and consistently working on balance exercises is a fundamental aspect of treatment. Cycling and swimming are beneficial for swelling reduction and increasing a patient’s cardiovascular fitness.
In the latter stages of rehabilitation, balance exercises should become more dynamic, including hopping and balancing on unstable surfaces, while whole leg strengthening should be incorporated.
Physiotherapy with James McCormack
This is not medical advice and we recommend a consultation with a medical professional such as James McCormack before trying any of these exercises. James offers Online Physiotherapy Appointments.
Related Articles:
Lateral Ankle Sprain Symptoms & Treatment – High Ankle Sprain – Medial Ankle Sprain