Read More >
- Anterior Ankle Impingement - July 24, 2022
- Tarsal Coalition - October 12, 2022
- Sural Nerve Pain - October 3, 2022
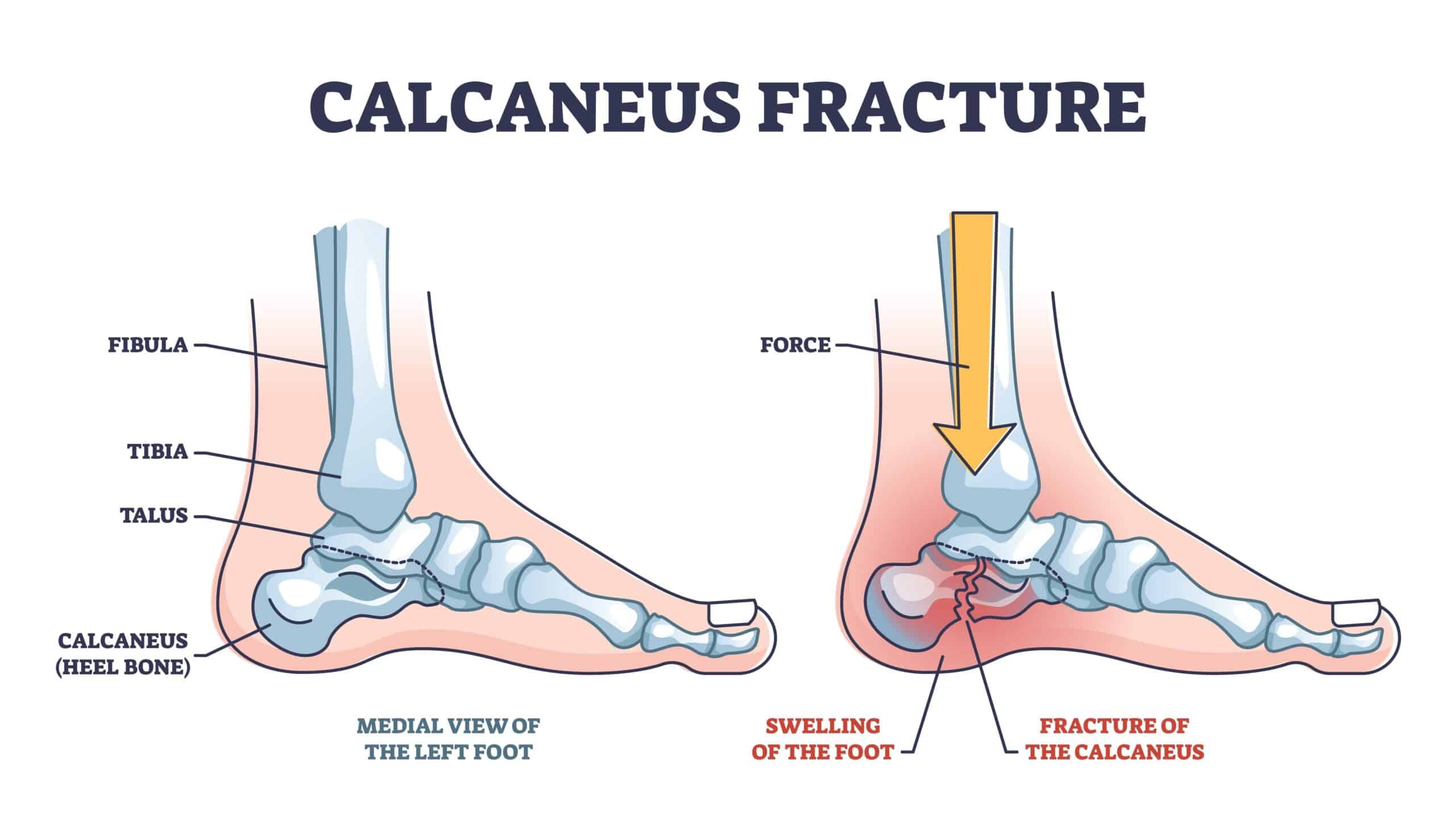
Calcaneus Anatomy
The Calcaneus bone (heel bone) sits on the base of the foot under the ankle joint, one of several tarsal bones, and along with the talus, it forms the hindfoot. Fracture to the calcaneus is rare, with tarsal bones accounting for approximately 2% of all fractures, while Calcaneus Fractures account for 50-60% of all tarsus fractures.
A fracture to the calcaneus is also known as a Lovers Fracture as historically it occurs when landing from a fall, i.e. jumping out of a window or off a balcony.
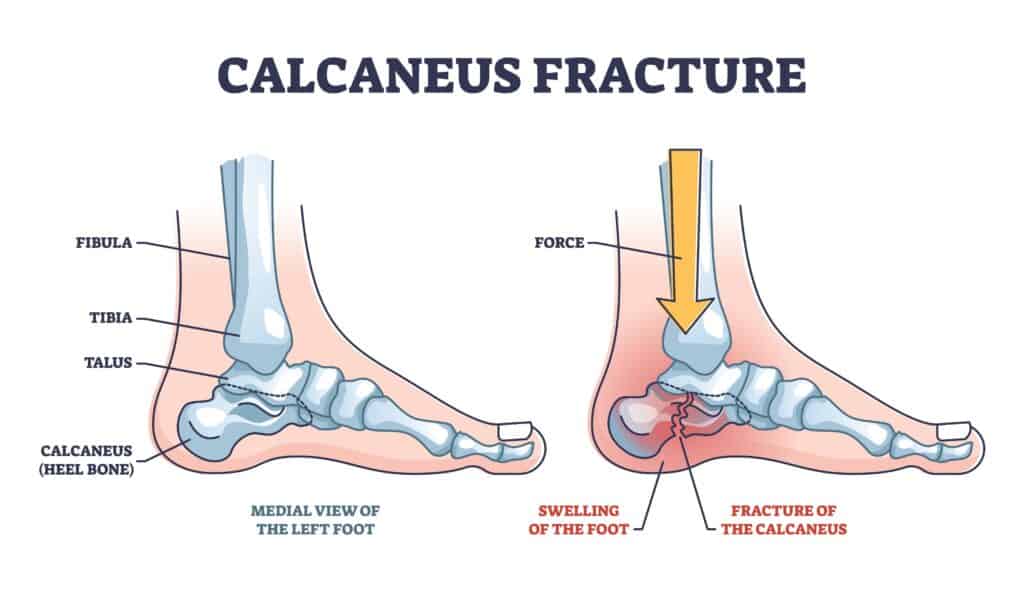
Calcaneus Fracture Symptoms
Symptoms of a Calcaneus Fracture include severe pain when weight bearing on the heel that is worse with impact activity such as walking, running or jumping.
A patient may notice swelling and heat around their heel bone, making it uncomfortable to wear tight-fitting shoes. Flat shoes with little cushioning are likely to aggravate the symptoms further.
In some cases, there may be swelling on the heel that can spread to the plantar surface of the midfoot.
Due to the intensity of pain and swelling, patients may walk on their forefoot to avoid placing pressure directly on the heel bone.

Causes of Calcaneus Fracture
The most common cause of a Calcaneus Fracture is a fall from a balcony, ladder, table or window. These high forces associated with landing from a height directly onto the Calcaneus are often sufficient to create an impact fracture. Similar types of Calcaneus Fractures can occur due to car crashes.
Repetitive stress on the Calcaneus bone from activities such as running can cause a Calcaneus Stress Fracture.
These types of stress fractures are often misdiagnosed as Insertional Achilles Tendonitis. Low Vitamin D levels, Osteopenia or Osteoporosis can increase your risk of developing a Calcaneus Stress Fracture.
Avulsion fractures are when a tendon or a ligament pulls off a fragment of bone from the Calcaneus.
This occurs from a sudden movement and typically involves the Achilles Tendon or the Bifurcate Ligament.
Calcaneus Fracture Diagnosis
A clinical assessment by a Physical Therapist can identify the likelihood of a Calcaneus Fracture through clinical tests such as the Calcaneal Squeeze test.
If this test is positive for pain, you will likely be referred for an x-ray.
If a Calcaneus Fracture is demonstrated on the x-ray, you may be referred for a CT scan for further clarity on the size and location of the fracture.
Calcaneus Fracture Classification
There are two main categories of Calcaneus Fracture. An extraarticular fracture accounts for 25% of all Calcaneus Fractures, while intraarticular fractures account for 75%.
Type 1
Fractures: Non-displaced or minimally displaced fragment
Type 2
2 bony fragments which are subdivided into A, B or C depending on if they are medial process or lateral process fracture
Type 3
3 bony fragments, divided into AB, AC or BC relative to the position and location of fracture lines
Type 4
4 comminuted bony fragments.
A Calcaneus Stress fracture can be caused by:
– High Impact Sports
– Overuse or overload
– Osteopenia or Osteoporosis
– History of stress fractures
– Relative energy deficiency in sport
Diagnosis in a clinical setting involves a thorough subjective assessment, while the Calcaneus Squeeze Test is a good clinical test. MRI is the gold standard form of imaging.
Depending on systemic health, treatment includes 4-6 weeks in a walker boot, identifying potential Biomechanical issues and a thorough strengthening programme.
Calcaneus Fracture Treatment
Treatment for Calcaneus Fracture is decided based on the type and location of the fracture. When conservative treatment is appropriate, a period of 4-6 weeks in a walker boot is recommended. Walking short distances in a boot as pain allows is usually recommended. After transitioning out of the walking boot, Physical therapy consisting of mobalisations, mobility and strengthening exercises should commence.
Physical Therapy can last 4-6 weeks, depending on the cause of injury. A fracture from a fall may require simple strengthening and rehabilitation. In contrast, a Calcaneus Stress Fracture from running can require a thorough gait analysis and running re-training alongside insoles and changes in footwear.
Surgery is necessary for a lot of instances of a Calcaneus Fracture. The type of surgery required should be discussed with an orthopaedic consultant.
Walking with a Calcaneus Fracture
If a Calcaneus fracture is treated conservatively, you can walk on it when wearing a walker boot as pain allows. The rocker sole and aircast protection of a walker boot facilitate a typical walking pattern for 5-10 minutes, but you should stop walking if you experience pain.
You will be guided by your therapist when you are allowed to begin walking in a regular shoe.
When can you return to running after a Calcaneus fracture?
If you have a Calcaneus fracture or broken heel, you can typically return to running after 12 weeks. The initial 4-6 weeks are spent in a walker boot, while the next 6 weeks are spent building up your strength and mobility with a Physical Therapist before returning to running.
Choosing cushioned footwear before returning to run is crucial as it helps to absorb the impact of heel strike.
Physiotherapy with James McCormack
This is not medical advice. We recommend a consultation with a medical professional such as James McCormack. He offers Online Physiotherapy Appointments weekly and appointments in his clinic in Fulham.