Plantar Fasciitis Brace
Read More >
The Plantar Fascia is a band of thick connective tissue that stretches across the plantar aspect (underneath) of the foot connecting the heel bone (calcaneus) and spanning across the foot to attach to the ball of the foot. The Plantar Fascia is a passive tissue that cannot contract like a muscle, but it plays a vital role in the structural integrity of the foot, provides stability to the arch of the foot and assists in the gait cycle.
When you stand, the foot spreads and stretches on the Plantar Fascia, while walking or running places a more significant strain on the tissue. The repetitive impact from running or having a flat foot can place excessive stress on the Plantar Fascia and cause a Plantar Fascia Tear.
A Plantar Fascia Tear can range from a small tear that is painful but has minimal effect on function to a full rupture to prevent weight bearing and significantly affect function levels. It is important to correctly identify a Plantar Fascia tear, as poor management could lead to the development of Pes Planus (Flat Feet).
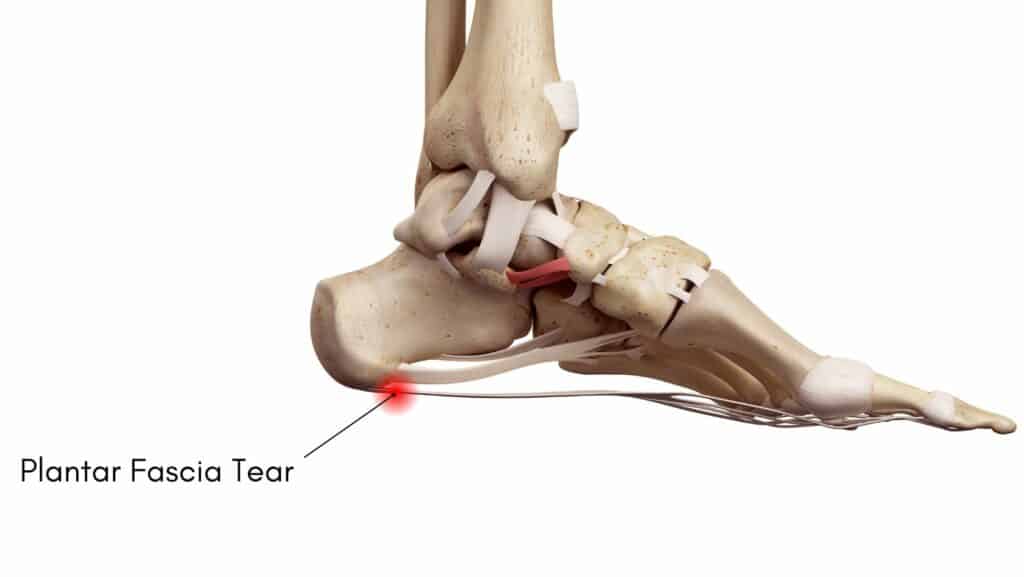
Plantar Fasciitis is the most well-known condition affecting the Plantar Fascia. It is essential to differentiate the symptoms of Plantar Fasciitis and a Plantar Fascia tear as their treatment differs considerably. The symptoms of a Plantar Fascia tear include a sharp immediate onset of pain when standing, walking or running. There can be an immediate onset of swelling and a bruise underfoot, while Plantar Fasciitis is usually slow and progressive in development with little to no swelling or bruising.
Typically Plantar Fasciitis provides stiffness on the heel when you first walk in the morning, which eases the more you walk, while a Plantar Fascia Tear is likely to worsen with increased walking.
The location of the pain varies depending on where the tear is located along the Plantar Fascia, but it is often very acute and localised to the tear. The tear is often incredibly tender to touch, and weight bearing may not be possible.

Steroid injections are the primary causes of a Plantar Fascia rupture.
These are prescribed for those with chronic Plantar Fasciitis as they can decrease pain levels and improve function, however, their use comes with an associated risk of rupture.
Plantar Fascia tears can occur from repetitive impact activities such as running and jumping, which are more common in the athletic population.
A Physical Therapist or a Sports Medicine Doctor can clinically diagnose a Plantar Fascia tear based on a patient’s symptoms and a Physical examination due to the stark differences in the onset of Plantar Fasciitis.
However, if a clinician would like to confirm the diagnosis or rule out other conditions, they are likely to refer a patient for an Ultrasound or an MRI.
An ultrasound is a cost-effective method of diagnosing a Plantar Fascia tear, while an MRI can give a more detailed image.
Initially, a severe Plantar Fascia tear is placed in a walker boot for 2-4 weeks to reduce inflammation and allow the Plantar Fascia time to heal before commencing Physical Therapy. Milder Plantar Facia tears can be managed with Plantar Fascia taping and relative rest.
Physical Therapy consists of a Physical Assessment to identify muscular weaknesses, tight tissues and balance deficits. These should then be addressed with a thorough rehabilitation protocol.
A gait analysis can identify biomechanical factors that may lead to the Plantar Fascia being overloaded when walking or running, followed by advice on the correct footwear and the necessity for insoles.
Conservative treatment is highly successful, and rarely any form of surgery is required for a Plantar Fascia Tear.
A torn plantar facia should be placed in a walker boot, and you can continue walking when wearing the boot. Once the boot is removed, a gradual increase in walking volume is recommended.
A torn Plantar Fascia takes 4-9 weeks to heal, with a study of 18 athletes with a torn Plantar Fascia returning to running after 9 weeks.
No, a Plantar Fascia Tear does not require surgery; it heals exceptionally well in a walker boot. Surgery may be required in very rare cases that don’t respond to conservative treatment.
This is not medical advice, and we recommend a consultation with a medical professional such as James McCormack. James offers Online Physiotherapy Appointments weekly.