Baker’s Cyst
- Outside Ankle Pain: Running, Standing, Walking - February 14, 2024
- Plantar Fasciitis Taping - January 30, 2024
- Peroneal Tendonitis Taping - January 30, 2024
What is a Baker’s Cyst
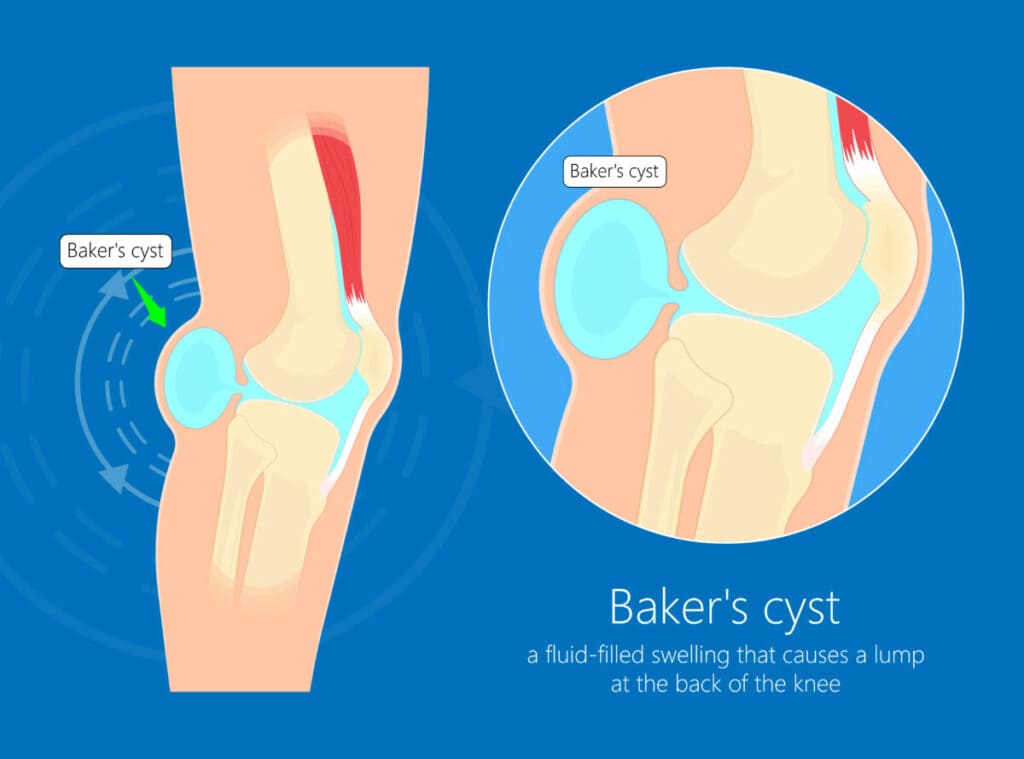
A Baker’s Cyst (Popliteal cyst) is a fluid collection at the back of the knee. This is generally due to pathology within the knee joint, such as a meniscus tear, that provokes excess fluid and knee pain.
It is pretty normal for the cyst to change in size daily, given that the amount of stress within the knee joint may vary depending on the activities carried out.
Is a Baker’s Cyst the main issue with my knee?
Not exactly. The palpable swelling of a Baker’s Cyst is usually the result of an intra-articular pathology of the knee. Meniscal tears, ACL injuries, different types of arthritis such as rheumatoid arthritis, and cartilage lesions are among the most prevalent diagnoses that could lead to a Baker’s cyst.
Symptoms?
The most typical symptom of a Baker’s Cyst is pain and swelling at the back of the knee. Generally, you should be able to palpate a small lump in the inner-posterior part of the joint.
Some positions or movements may be more uncomfortable than others due to excessive cyst compression, as in a deep squat and in bending the knee. However, also a prolonged period of standing may be uncomfortable.
Ruptured Bakers Cyst?
Yes, when excessive compression is applied to the cyst, for example, if you have been kneeling or squatting extensively, this may rupture the cyst and cause the fluid to leak into your calf muscles and ankle joint.
This may result in significant calf and ankle pain, swelling, and bruising. There may also be a notable difference in size between the two calves. This is generally not an important problem, as the swelling tends to reabsorb within a few weeks.
Elevating the leg and simple calf muscle pump exercises can be an excellent combination to help reduce the swelling faster.
Bakers Cyst Treatment
In most cases, conservative treatment such as physical therapy is warranted, along with addressing the underlying intra-articular cause of the cyst.
Hip-dominant exercises should be preferred over knee-dominant exercises due to the compressive action these may exert on the cyst.
Examples of good exercises for a Baker’s Cyst are:
- Single leg Deadlifts
- Crab walks
- Long lever bridges
- Side planks
- Resisted Leg Extension
- Straight Leg raise
Needle aspiration of the cyst and a corticosteroid injection may be helpful in the short term. However, if the underlying issue that caused a Baker’s Cyst to arise in the first place is not treated, the problem is likely to recur.
Baker’s Cyst activities to avoid?
As discussed above, a Baker’s Cyst tends to be compressed by knee-bending activities. Hence, squats, lunges, and hamstring curls should be avoided to prevent a premature cyst rupture.
If you are a keen cyclist, adjusting the height of your saddle may help reduce the amount of knee bending, thus making cycling less painful. Activities such as yoga, where one sits on one’s heels, should be avoided.
Lastly, due to the location of the cyst between the medial gastrocnemius (part of the calf muscles) and the semi-membranous (part of the hamstrings), forceful stretching of the hamstring and the calves should be avoided.
Baker’s Cyst in Children
Bakers cysts are common in children, especially boys between 4 and 8 years old. They may complain of a painless lump at the back of their knee, which fluctuates depending on their activity.
Unlike in adults, there is no apparent reason for the development of a Baker’s Cyst in children. This may sometimes become uncomfortable after a prolonged period of standing but will be generally pain-free for the rest of the time. Treatment is rarely necessary as the issue tends to resolve spontaneously.
How to Sleep with Baker’s Cyst?
Finding a comfortable position to sleep in can be difficult with a Baker’s cyst. Swelling at the back of the knee can compress the nerves and blood vessels at the back of the knee, and if these become compressed due to certain sleeping positions then it can become hard to sleep or wake you from your sleep.
In our experience, the best sleeping positions for a Baker’s Cyst are lying on your side with a pillow between your knees or lying on your back with cushioning behind the thigh and calf with a space behind the knee, to avoid any direct pressure.
Sleeping positions to avoid with a Baker’s Cyst are sleeping on your back with a pillow directly behind your knee or lying on your front with your knee fully extended. The direct pressure of a pillow behind the knee can cause compression and discomfort while lying on your front leading to tendon compression over the Baker’s cyst that can be uncomfortable when left in this position overnight.
__________________________________
We are specialists in treating foot conditions such as arthritis in the big toe joint and have experts in knee conditions in our clinic in Fulham, South West London. We also run a specialist Biomechanics and Custom Orthotics Service.
Related Articles:
Housemaid’s Knee – Exercises for Calf Strains – IT Band Syndrome
